Integrated and sequential screening
The integrated test is a method of screening for Down's syndrome which uses measurements obtained during the first and second trimesters of pregnancy to provide a single estimate of the risk of having a pregnancy with Down's syndrome.
The markers used in the Integrated test are maternal age with nuchal translucency and PAPP-A in the first trimester, and AFP, uE3, total or free ß hCG and inhibin-A in the second trimester. The Serum Integrated test omits the nuchal translucency measurement.
A significant improvement in screening performance can be achieved by adding the measurement of ductus venosus pulsatility index (DVPI), first trimester PlGF and a nasal bone examination (NBE) (see below).
Benefits of the Integrated Test
- A safe and effective method of screening for Down's Syndrome
- Screening performance similar to that reported for maternal plasma DNA sequencing methods
- Achieves a high detection rate with much lower false positive rate than other screening tests using maternal serum markers
- Preserves AFP screening for open neural tube defects
- Identifies pregnancies at high risk of trisomy 18 and trisomy 13, using first and second trimester serum markers, at high risk of SLOS using second trimester markers
- Requires fewer diagnostic procedures per case of Down's Syndrome detected than other screening tests
Screening Performance
The table below shows the estimated False Positive Rate at a 95% Detection Rate with first trimester markers measured at 11 completed weeks' gestation using the age distribution for England and Wales 2006-8 for the Integrated test, serum Integrated test, first trimester Combined test (nuchal translucency, total or free ß hCG and PAPP-A) , and the second trimester Quadruple test (AFP, uE3, total or free ß hCG and inhibin-A). The performance of the Integrated test and Combined test are shown with and without the measurement of DVPI, first trimester PlGF and a NBE. (See references 5,7,8 and 9)
Adding Ductus venosus pulsatility index, first trimester PlGF and a nasal bone examination to the Integrated test decreases the false positive rate at a 95% detection rate from 2,9% to 0.4% and to the Combined test decreases it from 13.3% to 2,2%.
The figure below shows a plot of the false-positive rate against detection rate for the four tests with the addition of the measurement of DVPI, first trimester PlGF and a NBE.
| Test | Additional Markers | False Positive Rate (%) at 95% detection rate |
| Integrated test | DVPI, first trimester PlGF and a NBE | 0.4 |
| Combined test | DVPI, first trimester PlGF and a NBE | 2.2 |
| Integrated test | None | 2.9 |
| Serum Integrated test | First trimester PlGF | 11.2 |
| Serum Integrated test | None | 12.4 |
| Combined test | None | 13.3 |
| Quadruple test | None | 15.7 |
Detection rate plotted against false-positive rate for the Combined (CT) and Integrated (IT) tests with the addition of first trimester ductus venosus pulsatility index (DVPI), nasal bone examination (NBE) and placental growth factor (PlGF), the serum integrated test (SIT) with the addition of second trimester PlGF and the Quadruple test (QT) with the addition of second trimester PlGF (first trimester markers measured at 11 completed weeks (from reference 5)

Sequential testing
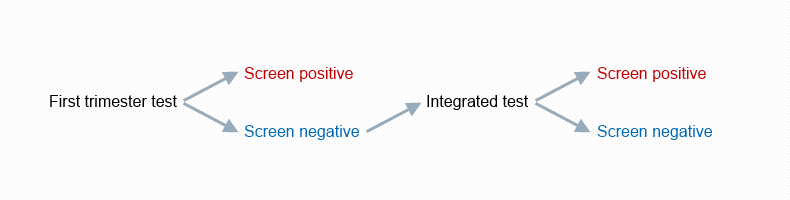
αlpha can be used to interpret sequential testing which allows early completion of screening for women with very high risk Down's syndrome, trisomy 18 or trisomy 13 pregnancies identified in the first trimester. A high risk cut-off (user defined) is set for the first trimester test so there is a low false positive rate. Nearly all women proceed to the full Integrated test. Information on pregnancies which are not positive are held for use in an Integrated test.
The figure below illustrates sequential testing.
More information
1.Integrated screening for Down's syndrome based on tests performed during the first and second trimesters (1999)
2.First and second trimester antenatal screening for Down’s syndrome: the results of the Serum, Urine and Ultrasound Screening Study (SURUSS) (2003)
3.SURUSS in perspective (2004)
4.Sequential and contingent prenatal screening for Down syndrome (2006)
5.Improvements in antenatal screening for Down’s syndrome (2013)
6.Sequential Integrated antenatal screening for Down’s syndrome, trisomy 18 and trisomy 13 (2015)
7.Prenatal screening for Down syndrome in twin pregnancies: Estimates of screening performance based on 61 affected and 7302 unaffected twin pregnancies (2018)
8.Corrigendum for Wald NJ, Bestwick JP, Huttly WJ, Aldis J, Borrell A, Goodburn S & Mills I (2018) https://doi.org/10.1002/pd.5381 (2019)
9.Antenatal screening for Down’s Syndrome: Revised nuchal translucency upper truncation limit due to improved precision of measurement (2020)